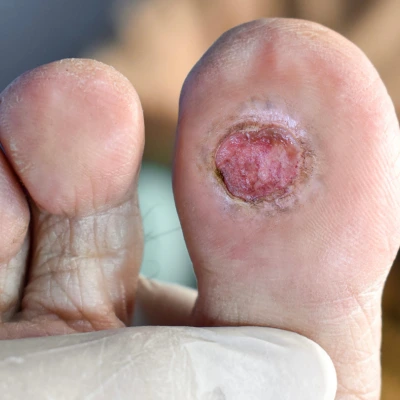
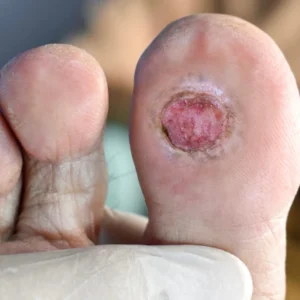
A diabetic foot ulcer is an open sore or wound that commonly occurs on the bottom of the foot in people with diabetes. High blood sugar levels can damage blood vessels and nerves over time, leading to poor circulation and loss of sensation in the feet. Because of this, small cuts, blisters, or injuries may go unnoticed and can develop into serious ulcers if not treated promptly.
Causes and Risk Factors
-
Nerve damage (diabetic neuropathy)
-
Poor blood circulation
-
Foot deformities or pressure points
-
Wearing ill-fitting shoes
-
Uncontrolled blood sugar levels
Symptoms to Watch For
-
Swelling, redness, or warmth in the foot
-
Persistent sores, cuts, or wounds that don’t heal
-
Drainage or foul odor from a wound
-
Black tissue (gangrene) in severe cases
Complications
If untreated, diabetic foot ulcers can lead to infections, tissue damage, or even amputation. That’s why early detection and proper care are critical.
Diagnosis and Treatment
Doctors may examine the wound, check blood flow, and test for infection. Treatment may include:
-
Wound cleaning and dressing
-
Medications for infection
-
Special footwear to reduce pressure on the ulcer
-
Blood sugar control to promote healing
-
Surgery in severe cases
Prevention Tips
-
Inspect your feet daily for cuts or blisters
-
Keep blood sugar under control
-
Wear comfortable, properly fitted shoes
-
Maintain good foot hygiene
-
Visit a podiatrist regularly
✅ Takeaway: Diabetic foot ulcers are preventable with proper foot care and diabetes management. If you notice any unusual wounds or changes in your feet, seek medical advice immediately to avoid complications.